The article summarizes the results of clinical and experimental studies of the formation of mandibular fractures of non-gunshot origin depending on the direction and angle of impact, the features of destruction of its surface during jaw clamping and unclamping. To conduct an experimental reproduction of mechanical blunt trauma of the mandible, to document the localization of fractures and to determine the potential relationship between the site of impact and the site of fracture to determine the nature of bone destruction depending on both the direction of impact and the state of functioning of the jaws. The study revealed a clear pattern. Namely, fractures were formed either in the area of impact to the lower jaw or in the area adjacent to the impact site. The number of fractures also varied depending on the impact site. In no case did a blow to the same area cause exactly the same type of fracture, and the location of fractures that occurred in areas other than the impact site also differed significantly in terms of the structural geometry of the mandible. The fractures occurred consistently in areas recognized as biomechanically weak, such as the necks of the articular and condylar processes, corners, and mental foramina. There was a difference between fractures in closed and open jaws. Thus, with closed jaws, fractures from direct compression are formed on the outer surface of the jaw, and on the inner surface - tension, where the primary fracture is formed, and a bone fracture zone is formed at the site of direct contact. On the contrary, when the jaws are open, indirect fractures are formed on the opposite side. That is, when diagnosing non-gunshot fractures of the mandible, it is necessary to take into account not only the force of impact, its direction, but also the condition of the masticatory muscles during the injury and the position of the victim's head.
| Published in | International Journal of Dental Medicine (Volume 11, Issue 1) |
| DOI | 10.11648/j.ijdm.20251101.15 |
| Page(s) | 34-40 |
| Creative Commons |
This is an Open Access article, distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution and reproduction in any medium or format, provided the original work is properly cited. |
| Copyright |
Copyright © The Author(s), 2025. Published by Science Publishing Group |
Mandible, Anatomical Features, Non-Gunshot Fracture, Localization, Displacement of Fragments
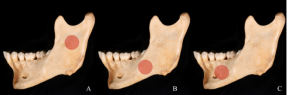
Sample | Value location | Number of fractures | Fracture Locations |
|---|---|---|---|
1 | Midline | 5 | Left and right articular processes; left and right body; symphysis |
2 | Midline | 4 | Right body; symphysis; left coronoid process; left articular process |
3 | Midline | 3 | Left and right articular process; symphysis |
4 | Front body | 2 | Right articular process; left anterior transition zone (body left) |
5 | Front body | 1 | Body and angle of the jaw on the left |
6 | Middle body | 1 | Body on the left |
7 | Middle body | 1 | Jaw angle on the left |
8 | Rear body | 1 | Left posterior transition zone (left corner) |
9 | Rear body | 2 | Jaw angle on the left; symphysis |
10 | Jaw branch | 3 | Jaw body right; left anterior transition zone (symphysis); left articular process |
11 | Jaw branch | 2 | Left anterior transition zone (jaw body left); left articular process |
AOCMF | Craniomaxillofacial Division of the AO Foundation |
The AO | Foundation is a Medically Guided, Not-For-profit Organization Led by an International Group of Surgeons Specialized in the Treatment of Trauma and Disorders of the Musculoskeletal System |
| [1] | Boffano P., Kommers S. C., Karagozoglu K. H., Gallesio C., Forouzanfar T. (2015). Mandibular trauma: a two-centre study. International journal of oral and maxillofacial surgery, issue 44, vol. 8, pp. 998–1004. |
| [2] | Bormann, K. H., Wild, S., Gellrich, N. C., Kokemüller, H., Stühmer, C., Schmelzeisen, R., & Schön, R. (2009). Five-year retrospective study of mandibular fractures in Freiburg, Germany: incidence, etiology, treatment, and complications. Journal of oral and maxillofacial surgery: official journal of the American Association of Oral and Maxillofacial Surgeons, issue 67, vol. 6, pp. 1251–1255. |
| [3] | Carvalho, T. B., Cancian, L. R., Marques, C. G., Piatto, V. B., Maniglia, J. V., & Molina, F. D. (2010). Six years of facial trauma care: an epidemiological analysis of 355 cases. Brazilian journal of otorhinolaryngology, issue 76, vol. 5, pp. 565-574. |
| [4] | Rashid, A., Eyeson, J., Haider, D., van Gijn, D., & Fan, K. (2013). Incidence and patterns of mandibular fractures during a 5-year period in a London teaching hospital. The British journal of oral & maxillofacial surgery, issue 51, vol. 8, pp. 794-798. |
| [5] | Matsyuk D., Kuzniak N. (2024). Clinical analysis of the location, nature and type of mandibular fractures in patients on admission to hospital Intermedical journal, vol. 1, pp. 134-139. |
| [6] | Mihajlichenko B. V., Bilyakov A. M., Franchuk V. V. (2024). Sudova stomatologiya [Judicial dentistry]: pidruchnik. K.: VSV «Medicina». 263 p. ISBN 978-617-505-977-7 |
| [7] | Jung, H. W., Lee, B. S., Kwon, Y. D., Choi, B. J., Lee, J. W., Lee, H. W., Moon, C. S., & Ohe, J. Y. (2014). Retrospective clinical study of mandible fractures. Journal of the Korean Association of Oral and Maxillofacial Surgeons, issue 40, vol. 1, pp. 21-26. |
| [8] | Kaura, S., Kaur, P., Bahl, R., Bansal, S., & Sangha, P. (2018). Retrospective Study of Facial Fractures. Annals of maxillofacial surgery, issue 8, vol. 1, pp. 78-82. |
| [9] | Ali Ghalib Mutar Mahdi, Issam Abdul Aziz Ali (2013). A retrospective analytic study of mandibular fracture patterns in two different periods in Baghdad, Journal of Oral and Maxillofacial Surgery, Medicine, and Pathology, issue 3, vol. 25, pp. 205-209. |
| [10] | Fang, C. Y., Tsai, H. Y., Yong, C. Y., Ohiro, Y., Chang, Y. C., & Teng, N. C. (2023). A 10-year retrospective study on mandibular fractures in Northern Taiwan. Journal of dental sciences, issue 18, vol. 3, pp. 1330–1337. |
| [11] | Brechlychuk P. P., Goncharuk-Khomyn M. Y. (2019). Estimation of the mandible fracture pattern according to retrospective studies with a large amount of studied samples. Clinical dentistry. vol. 1, pp. 11-18. |
| [12] | Subhashraj, K., Ramkumar, S., & Ravindran, C. (2008). Pattern of mandibular fractures in Chennai, India. The British journal of oral & maxillofacial surgery, issue 46, vol. 2, pp. 126–127. |
| [13] | Sinha, V., Chaudhary, N., Jha, S. G., Chaudhari, N. P., & Rathva, K. R. (2022). Management of Maxillofacial Trauma in Road Traffic Accident (RTA) at Tertiary Care Center. Indian journal of otolaryngology and head and neck surgery: official publication of the Association of Otolaryngologists of India, issue 74, vol. 2, pp. 1246-1252. |
| [14] | Unnewehr, M., Homann, C., Schmidt, P. F., Sotony, P., Fischer, G., Brinkmann, B., Bajanowski, T., & DuChesne, A. (2003). Fracture properties of the human mandible. International journal of legal medicine, issue 117, vol. 6, pp. 326-330. |
| [15] | Panesar, K., & Susarla, S. M. (2021). Mandibular Fractures: Diagnosis and Management. Seminars in plastic surgery, issue 35, vol. 4, pp. 238-249. |
| [16] | Farzan, R., Farzan, A., Farzan, A., Karimpour, M., & Tolouie, M. (2021). A 6-Year Epidemiological Study of Mandibular Fractures in Traumatic Patients in North of Iran: Review of 463 Patients. World journal of plastic surgery, issue 10, vol. 1, pp. 71-77. |
| [17] | Shetty, V., Atchison, K., Der-Matirosian, C., Wang, J., & Belin, T. R. (2007). The mandible injury severity score: development and validity. Journal of oral and maxillofacial surgery: official journal of the American Association of Oral and Maxillofacial Surgeons, issue 65, vol. 4, pp. 663-670. |
| [18] | Yunus, A. D., Gultom, F. P., Puspitawati, R., Sari, F. A., Prastyo, E., Rijaldi, F., & Suripto, S. (2024). Dental Profiling and Findings of Multiple Jaw Fractures in Traffic Accident Victim: A Case Report. E-GiGi, issue 12, vol. 2, pp. 246-252. |
| [19] | Fenton, T. W., Birkby, W. H., & Cornelison, J. (2003). A fast and safe non-bleaching method for forensic skeletal preparation. Journal of forensic sciences, issue 48, vol. 2, pp. 274-276. |
| [20] | Isa, M. I., Fenton, T. W., Goots, A. C., Watson, E. O., Vaughan, P. E., & Wei, F. (2019). Experimental investigation of cranial fracture initiation in blunt human head impacts. Forensic science international, vol. 300, pp. 51-62. |
| [21] | Goots, A., Isa, M. І., Fenton, T. W., Wei, F. (2022). Blunt force trauma in the human mandible: An experimental investigation. Forensic Science International 5 100252 |
| [22] | Kaye B., Randall C., Walsh D., & Hansma P. (2012). The effects of freezing on the mechanical properties of bone, Open Bone J., vol. 4, pp. 14-19. |
| [23] | Cornelius, C. P., Audigé, L., Kunz, C., Rudderman, R., Buitrago-Téllez, C. H., Frodel, J., & Prein, J. (2014). The Comprehensive AOCMF Classification System: Mandible Fractures- Level 2 Tutorial. Craniomaxillofacial trauma & reconstruction, issue 7, vol. 1, pp. 15-30. |
| [24] | Cornelius, C. P., Audigé, L., Kunz, C., Rudderman, R., Buitrago-Téllez, C. H., Frodel, J., & Prein, J. (2014). The Comprehensive AOCMF Classification System: Mandible Fractures-Level 3 Tutorial. Craniomaxillofacial trauma & reconstruction, issue 7, vol. 1, pp. 31-43. |
| [25] | Viano, D. C., Bir, C., Walilko, T., & Sherman, D. (2004). Ballistic impact to the forehead, zygoma, and mandible: comparison of human and frangible dummy face biomechanics. The Journal of trauma, issue 156, vol. 6, pp. 1305–1311. |
| [26] | Craig, M., Bir, C., Viano, D., & Tashman, S. (2008). Biomechanical response of the human mandible to impacts of the chin. Journal of biomechanics, issue 141, vol. 14, pp. 2972–2980. |
| [27] | Zhou, H., Lv, K., Yang, R., Li, Z., & Li, Z. (2016). Mechanics in the Production of Mandibular Fractures: A Clinical, Retrospective Case-Control Study. PloS one, issue 11, vol. 2, p. 0149553. |
APA Style
Oleksandr, B., Oleksandra, R., Natalia, B., Mykola, S., Vugar, A. (2025). Experimental Modelling of Non-Gunshot Fractures of the Mandible. International Journal of Dental Medicine, 11(1), 34-40. https://doi.org/10.11648/j.ijdm.20251101.15
ACS Style
Oleksandr, B.; Oleksandra, R.; Natalia, B.; Mykola, S.; Vugar, A. Experimental Modelling of Non-Gunshot Fractures of the Mandible. Int. J. Dent. Med. 2025, 11(1), 34-40. doi: 10.11648/j.ijdm.20251101.15
AMA Style
Oleksandr B, Oleksandra R, Natalia B, Mykola S, Vugar A. Experimental Modelling of Non-Gunshot Fractures of the Mandible. Int J Dent Med. 2025;11(1):34-40. doi: 10.11648/j.ijdm.20251101.15
@article{10.11648/j.ijdm.20251101.15,
author = {Belikov Oleksandr and Roshchuk Oleksandra and Belikova Natalia and Sorokhan Mykola and Aliyev Vugar},
title = {Experimental Modelling of Non-Gunshot Fractures of the Mandible
},
journal = {International Journal of Dental Medicine},
volume = {11},
number = {1},
pages = {34-40},
doi = {10.11648/j.ijdm.20251101.15},
url = {https://doi.org/10.11648/j.ijdm.20251101.15},
eprint = {https://article.sciencepublishinggroup.com/pdf/10.11648.j.ijdm.20251101.15},
abstract = {The article summarizes the results of clinical and experimental studies of the formation of mandibular fractures of non-gunshot origin depending on the direction and angle of impact, the features of destruction of its surface during jaw clamping and unclamping. To conduct an experimental reproduction of mechanical blunt trauma of the mandible, to document the localization of fractures and to determine the potential relationship between the site of impact and the site of fracture to determine the nature of bone destruction depending on both the direction of impact and the state of functioning of the jaws. The study revealed a clear pattern. Namely, fractures were formed either in the area of impact to the lower jaw or in the area adjacent to the impact site. The number of fractures also varied depending on the impact site. In no case did a blow to the same area cause exactly the same type of fracture, and the location of fractures that occurred in areas other than the impact site also differed significantly in terms of the structural geometry of the mandible. The fractures occurred consistently in areas recognized as biomechanically weak, such as the necks of the articular and condylar processes, corners, and mental foramina. There was a difference between fractures in closed and open jaws. Thus, with closed jaws, fractures from direct compression are formed on the outer surface of the jaw, and on the inner surface - tension, where the primary fracture is formed, and a bone fracture zone is formed at the site of direct contact. On the contrary, when the jaws are open, indirect fractures are formed on the opposite side. That is, when diagnosing non-gunshot fractures of the mandible, it is necessary to take into account not only the force of impact, its direction, but also the condition of the masticatory muscles during the injury and the position of the victim's head.
},
year = {2025}
}
TY - JOUR T1 - Experimental Modelling of Non-Gunshot Fractures of the Mandible AU - Belikov Oleksandr AU - Roshchuk Oleksandra AU - Belikova Natalia AU - Sorokhan Mykola AU - Aliyev Vugar Y1 - 2025/05/09 PY - 2025 N1 - https://doi.org/10.11648/j.ijdm.20251101.15 DO - 10.11648/j.ijdm.20251101.15 T2 - International Journal of Dental Medicine JF - International Journal of Dental Medicine JO - International Journal of Dental Medicine SP - 34 EP - 40 PB - Science Publishing Group SN - 2472-1387 UR - https://doi.org/10.11648/j.ijdm.20251101.15 AB - The article summarizes the results of clinical and experimental studies of the formation of mandibular fractures of non-gunshot origin depending on the direction and angle of impact, the features of destruction of its surface during jaw clamping and unclamping. To conduct an experimental reproduction of mechanical blunt trauma of the mandible, to document the localization of fractures and to determine the potential relationship between the site of impact and the site of fracture to determine the nature of bone destruction depending on both the direction of impact and the state of functioning of the jaws. The study revealed a clear pattern. Namely, fractures were formed either in the area of impact to the lower jaw or in the area adjacent to the impact site. The number of fractures also varied depending on the impact site. In no case did a blow to the same area cause exactly the same type of fracture, and the location of fractures that occurred in areas other than the impact site also differed significantly in terms of the structural geometry of the mandible. The fractures occurred consistently in areas recognized as biomechanically weak, such as the necks of the articular and condylar processes, corners, and mental foramina. There was a difference between fractures in closed and open jaws. Thus, with closed jaws, fractures from direct compression are formed on the outer surface of the jaw, and on the inner surface - tension, where the primary fracture is formed, and a bone fracture zone is formed at the site of direct contact. On the contrary, when the jaws are open, indirect fractures are formed on the opposite side. That is, when diagnosing non-gunshot fractures of the mandible, it is necessary to take into account not only the force of impact, its direction, but also the condition of the masticatory muscles during the injury and the position of the victim's head. VL - 11 IS - 1 ER -